Life, the Vagus Nerve and HRV
The connection between Life, the Vagus Nerve and HRV. With apologies to Douglas Adams.
Life. What is the drive that appears to be so pervasive as part of the human condition? Does the Vagus Nerve and Heart Rate Variability (HRV) give us insight into life and the health not just of our bodies but of our minds?
In two to three generations Western societies have gone from having to boil water for a bath and hunt animals for subsistence to having hot water, refrigeration, transport and endless entertainment on tap, not to mention processed food we don’t need to leave home for. Ironically, hunting for food and bathing outside is now a luxury afforded only by the rich. We are in clover.
Yet, we still strive for more in life. What is this life force that drives us? Is it just longevity or are we driven by well-being or a life well-lived?
In 1969, Lawrence LeShan a prominent psychologist stated that “we have not as yet found a useful way of conceptualizing the life and death forces within the individual.”1 However, he goes on to state, that the “ideal of the full rich self, the development of ones own being in one’s own special way, the freedom to be oneself fully without fear – this is the goal acceptable to our Zeitgeist and worth fighting and suffering for.” In my observation of patients over many years, those who look back on a live well lived are paradoxically more able to accept it’s ending.
Purpose in life, defined as “a self-organizing life aim that stimulates goals, promotes healthy behaviors and gives meaning to life” is associated with longevity.2 Furthermore, psychological well-being is associated with improved current physical health and function.3 It appears that positive re-reinforcement is in place in the human organism. A purpose in life leads to healthy behaviors and healthy behaviors support purpose. The practice of religion, pursuing altered consciousness by means including extreme sports, substance use and meditation, and striving to make a difference, bear witness to the human drive for more. Ignoring this part of human nature leads to poor physical health. It is as if the life force, being neglected, slowly leaves.
Moving to 2020, it appears that science is still unable to construct a measurement for happiness and purpose, instead using questionnaires and measuring physical health outcomes in relation to the concept of well-being. A Pubmed search using “life-force” as a search term brings up papers on managing obesity, homeopathy and attempting to turn a strand of DNA into life. However, despite reductionist specialty and Descarte’s separation of mind and body, the Hippocratic view of a body-mind continuum is slowly reappearing in medical research.4
No separation of mind and body exists, nor has a pathway of consciousness every been found. Interested readers can delve into Stainslav Grof’s writing regarding trans-personal consciousness amongst other influencing factors on an individual’s well-being. Increasing research postulates that the Vagus Nerve and it’s effect on the heart and the rest of body is the “missing link” between the mind and the body.5 The output of the Vagus Nerve, as measured by Heart Rate Variability (HRV), links the physical state and function of the organism with its responses to physical, emotional and cognitive stimulation, influencing longevity. Additionally, it is known that the community and environment have an impact on an individual’s health and Vagus nerve.6
In layman’s terms, all life is connected and directly affects the health and well-being of the individual. The health status of the individual influences their life-choices (such as diet, movement and substance use), social engagement and environmental connection. These in turn feed back to the individual, whether positively or negatively.
The question then is: Can we know if we are supporting our life force? My answer is a resounding yes. Measure where the mind and body coalesce: the heart. In particular measure Heart Rate Variability.
For centuries the heart has been considered the source of emotion, courage and wisdom.7 However, in medical school, we were taught of a mechanical pump that got it’s instructions from the brain on how hard and fast to beat. Nothing could be further from the truth and this was known by the time I went to medical school;8 but as they say, it takes the passing of a generation of academics for new research to be accepted.
The heart not only has its own neural network, called the Intrinsic Cardiac Nervous System or Heart-Brain, but also directly communicates with the brain. In fact, the heart sends more messages to the brain than the brain sends to the heart. These messages from the heart reach the brain stem and then the cortex, where we process information and make decisions. Your heart most certainly affects your choices in life, influencing attention level, motivation, and emotional processing.7
Of interest, the gut too, has its own neural network, called the Enteric Nervous System or Gut-Brain, which communicates directly with the brain. Integrating the gut-brain, heart-brain and head-brain is a method used to support decision making and intuition.7
Heart Rate Variability (HRV) and the Vagus Nerve in Life
The Autonomic Nervous System (ANS) automatically controls the body’s internal functions. You do not need to think about digesting, breathing or lowering and raising your heart rate. The ANS does this for you. The ANS, in turn, is a balance of the Parasympathetic (rest and digest) and Sympathetic (fight, flight, or freeze) nervous systems.
In the ANS, the Vagus nerve, stands out as the main controller and is reflected in life by HRV. It is part of the Parasympathetic (rest and digest) system and is the longest cranial nerve, starting in the brain stem and sending out nerves to the heart, liver, kidneys, pancreas, esophagus, intestines, and throat. The Vagus nerve forms part of the heart’s neural communication to the brain.
It is thought that the Vagus nerve was central to the development of emotional responses in the evolution of humans.7 It is often described as the Vagus break on the Sympathetic (fight, flight, freeze) system. As humans we can self-regulate and calm the Sympathetic response. We do this mainly through the Vagus nerve. If we were under constant Sympathetic dominance our lives would be short and sharp indeed. We have our Vagus nerves to thank for our humanity.
We have our Vagus nerves to thank for our humanity
Measurement of the Vagus nerve activity is thus a reflection of the individual’s ability to self-regulate and by extension live a long and healthy life. Indeed, those with the highest self-regulatory abilities were over 50 times more likely to be alive and without chronic disease 15 years later, than those with the lowest self-regulation scores.5 To quote William Osler one of the founders of Johns Hopkins Hospital: “It is very often much more important what person has the disease than what disease the person has.”
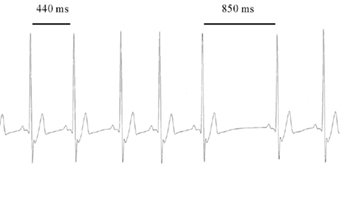
One of the main ways that the Vagus nerve’s influence in life can be measured is through Heart Rate Variability (HRV). HRV is the measure of the normally occurring beat-to-beat changes in heart rate. An optimal HRV reflects healthy function, capacity, and adaptability of the individual.6
Multiple mathematical measurements of HRV are in use and reflect subtly different aspects of the Vagus nerve and ANS. It is important to note that HRV is not a static measure. While HRV naturally decreases with age, a higher HRV generally indicates greater health and potential lifespan, while a lower HRV indicates the opposite.
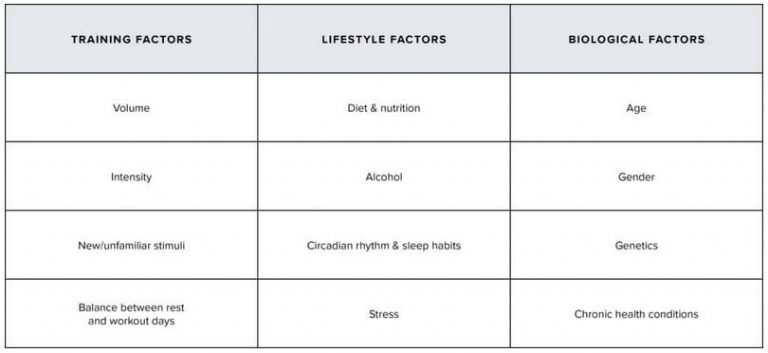
Day to day HRV measurements can be used to assess the body’s response to challenges such as physical training or emotional stressors. Your HRV should drop after an intense training session and then slowly rise back again, possibly settling higher than before the training. Similarly, if you are fighting a virus, under emotional stress or dehydrated, your HRV is likely to drop. On the flip side, if you never challenge your body or mind with learning, striving or physical training, your HRV may just slowly drop with age, along with your life-force.
Of interest is the effect of daily habits on HRV. I particularly notice how alcohol, or a late meal will significantly drop my HRV. This proves to be a potent motivator. The effect of training and alcohol on HRV in a cohort of over 57000 people was recently explored, confirming the use of HRV as a means to identify health and lifestyle effects for individuals and across populations.9
Looking at general health, a decrease in Vagus nerve output (low HRV) is associated with increased inflammation, insulin resistance, atherosclerosis6, depression and anxiety,10 as well as bowel, digestive, immune and cognitive health.11 Vagus nerve stimulation (and thus a higher HRV) is associated with neuroprotective effects.12 The Vagus nerve has been described as a tranquilizer, slowing down the beat-to-beat heart intervals and improving HRV and thus life.13
Furthermore, HRV has been suggested as a means to assess drug and lifestyle therapies in relation to mortality and prognosis.14
You can actively engage with and stimulate your Vagus nerve, improving your HRV and your life force. HRV is known to be increased by exercise, vegetable intake, positive social ties, spending time in nature and sufficient sleep.6 Biofeedback programs and regular breathing exercises such as alternate nostril breathing15 and rhythmic breathing at a rate of 6 breaths / minute16 will over time improve HRV. Interestingly rhythmically reciting a prayer or mantra has a similar effect.17
While only a few studies have looked directly at the effect of supplementation on HRV, those that did show a positive effect include: Fish oil,18 Vitamin B12,19 Magnesium20 and Co-enzyme Q-10 when used with exercise.21 Diffusing Japanese cedar essential oil is another way to support the Vagus nerve.22
Negative emotions, smoking, alcohol consumption and a perception of inequality will decrease HRV,6 as will air pollution23 and nutrient deficiencies.24
The Vagus nerve appears to promote our capacity for connecting with others
Of particular relevance to COVID-19, is the report that lack of social ties are associated with a 50% increased risk of early death across all ages over the following 7.5 year period.25 This is higher than the effect of smoking and it appears to be higher than the global population mortality rate of COVID-19.
HRV as a metric of our purpose
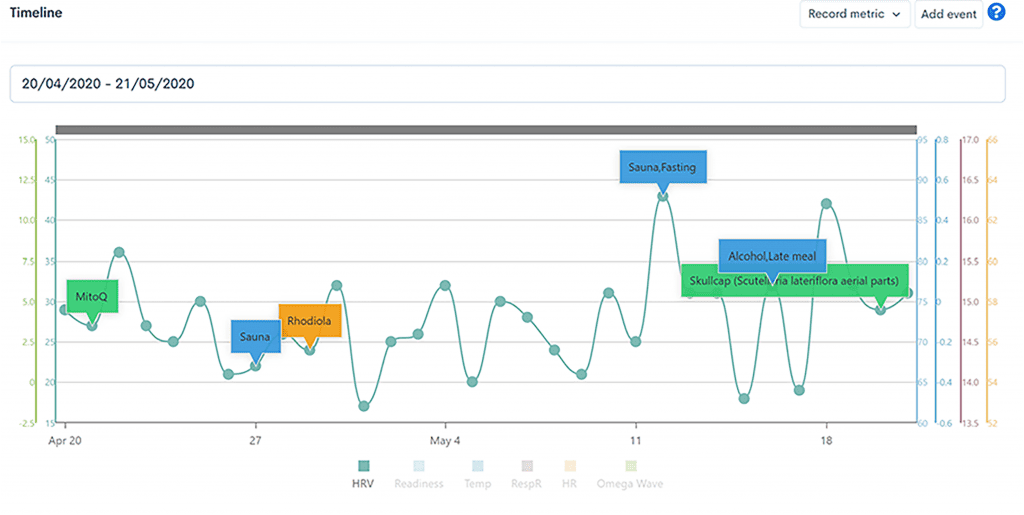
Dr Andrew Kemp and his team at Swansea University, have published extensively on the relationship between emotion, physical health and longevity,26 using HRV as a measurement of this integration.4 I have drawn heavily on their work both in the clinic and in my own life. They have suggested that Vagus nerve function (HRV) affects and is affected by “psychological experience, health behaviours, social ties, as well as the environment”, and the Vagus nerve is seen as the structural link between physical and mental health.6
In all due respect, I suggest that we take this measure further. While it may be premature to use HRV as a measure of life-force, given the role of the heart in our lives and the Vagus nerve’s role in our humanity, their coalescence in Heart Rate Variability may indeed be a metric of the essence of our lives, our will to live and our desire to thrive.